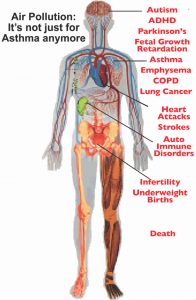
Particulate Matter
The Dangers of Particulate Matter Pollution
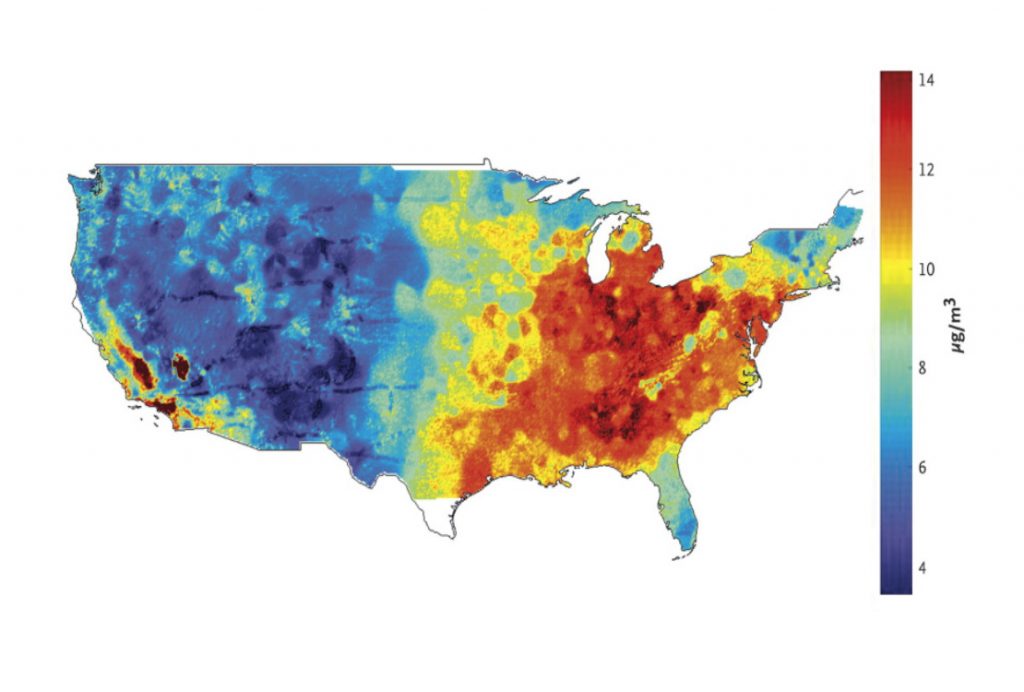
Most of the time, “Particulate Matter Pollution” is just another name for “soot,” exactly the kind of burnt, dusty remains of a fire that chimney sweeps got paid to clean-up in Mary Poppins. Fireplaces create it. So do gas and diesel engines, and industrial furnaces and boilers in power plants and cement kilns. Any process using fire or combustion makes soot.

When it gets studied by science, “soot” becomes “Particulate Matter,” and gets classified by size. There’s “PM10,” and “PM2.5.” The numbers refer to the diameter of the soot particle in microns, or one millionth of a meter. A human hair is usually around 50-70 microns across, but those follicles are giant redwoods compared to a piece of PM 10. When put next to soot only 2.5 microns in diameter or less, the differences are even more startling. It’s impossible to even see this kind of soot, so it’s called “ultra fine particles” or “micro particles.”
Its small size is what makes industrial PM pollution so dangerous to 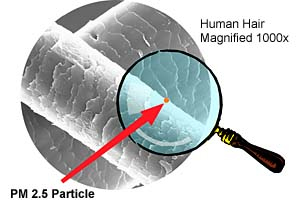 people. Evolution equipped us with filters in our nose and throat to catch larger, natural dust particles. But PM pollution is so tiny it slips right by these evolutionary safeguards and gets inhaled deep within our lungs. There, it’s small enough to pass through the lungs’ lining directly into our blood stream and deposit itself in other organs. This makes it toxic from the start.
people. Evolution equipped us with filters in our nose and throat to catch larger, natural dust particles. But PM pollution is so tiny it slips right by these evolutionary safeguards and gets inhaled deep within our lungs. There, it’s small enough to pass through the lungs’ lining directly into our blood stream and deposit itself in other organs. This makes it toxic from the start.
 Then the damage is compounded. Another difference between PM pollution and dust is that PM carries the residues of whatever was burned when it was made. Every piece of soot acts like a tiny suitcase – chock full of charred remnants of other chemicals. If the PM is coming out of a car or truck engine, it’ll have residues of Benzene and other hydrocarbons in it. If it’s coming out of coal-fired power plant, it will likely be stowing away some Mercury. If it’s coming out of a cement kiln that burns plastics or other industrial wastes, it might have some added Dioxin attached to it. This toxic hitchhiking is the second punch to our health when we inhale PM.
Then the damage is compounded. Another difference between PM pollution and dust is that PM carries the residues of whatever was burned when it was made. Every piece of soot acts like a tiny suitcase – chock full of charred remnants of other chemicals. If the PM is coming out of a car or truck engine, it’ll have residues of Benzene and other hydrocarbons in it. If it’s coming out of coal-fired power plant, it will likely be stowing away some Mercury. If it’s coming out of a cement kiln that burns plastics or other industrial wastes, it might have some added Dioxin attached to it. This toxic hitchhiking is the second punch to our health when we inhale PM.
Science has studied PM pollution for a long time, but other kinds of air  pollution, like smog, have often eclipsed it in notoriety and attention. Only now are we beginning to get a bigger, fuller picture of its impacts to human health. One of the most important new findings is that, like lead and other industrial toxins, there is no “safe level” of exposure to PM pollution for people. That is, inhaling any amount is capable of leaving some adverse health impact behind. This is especially true if you’re a child, a senior, or someone with existing respiratory problems.
pollution, like smog, have often eclipsed it in notoriety and attention. Only now are we beginning to get a bigger, fuller picture of its impacts to human health. One of the most important new findings is that, like lead and other industrial toxins, there is no “safe level” of exposure to PM pollution for people. That is, inhaling any amount is capable of leaving some adverse health impact behind. This is especially true if you’re a child, a senior, or someone with existing respiratory problems.
In the largest effort of its kind, a nationwide study of more than 60 million senior citizens published in 2017 linked long-term exposure to PM pollution to thousands of premature deaths annually, even at levels well below the legal limits set by the U.S. Environmental Protection Agency. The analysis found no sign of a “safe” level of pollution, below which the risk of dying early tapered off.
A second recent paradigm-shifting discovery about PM is the connection to unexpected illnesses.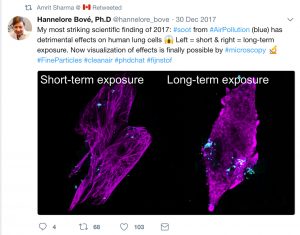
There’s now a substantial body of studies associating PM exposure to neurological diseases. In 2014, Harvard scientists found women exposed to higher levels of fine particulate matter during pregnancy may face up to twice the risk of having a child with autism than mothers living in areas with low particulate matter exposure. In 2013, USC researchers had concluded the same thing based on the proximity of pregnant women living near freeways. PM exposure has also been tied to attention deficit hyperactivity disorder, or ADHD, in children.
Some of the same kinds of health impacts have been noticed at the other end of the age spectrum. Exposure to PM pollution has been tied to Parkinson’s Disease, Dementia, Alzheimer’s, and general “cognitive decline” in adults. PM has also been linked to immune and reproductive system damage.
Combining its small size with its potent toxicity and access to any part of 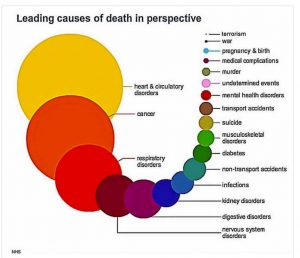 the body, PM pollution is probably the single most harmful kind of air pollution, capable of causing a wide range of health impacts – from life-long learning problems to death. Worldwide, PM pollution is estimated to cause about 25% of lung cancer deaths, 8% of COPD deaths, and about 15% of ischemic heart disease and stroke. No study has attempted to estimate the total public health damage to non cardiovascular organs and systems.
the body, PM pollution is probably the single most harmful kind of air pollution, capable of causing a wide range of health impacts – from life-long learning problems to death. Worldwide, PM pollution is estimated to cause about 25% of lung cancer deaths, 8% of COPD deaths, and about 15% of ischemic heart disease and stroke. No study has attempted to estimate the total public health damage to non cardiovascular organs and systems.
Not surprisingly, protections from PM pollution have not kept up with the science.
National air-quality standards for PM were first established in 1971 and were not significantly revised until 1987 when EPA changed the focus to “inhalable particles.” Since then, the federal ambient air standard for PM has been revised three times – all downward. In 2012, and again in 2019 the mandated-by-law EPA review didn’t include any of the most recent research tying the pollutant to neurological harms or studies finding those and other harms occurring well below the current EPA standard.
If we’re going to reduce the immense public health damage of air pollution, mere compliance with the federal standard for PM pollution isn’t going to be enough. We must reduce Particulate Matter pollution as much as possible from as many sources as possible.
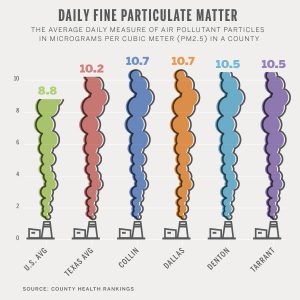
PM Pollution in North Texas
Unlike smog, DFW has never been in violation of a national standard for PM pollution. But that doesn’t mean the region doesn’t have a PM problem.
For years, annual PM levels in DFW flirted with what is now the annual standard. More recent readings show a leveling off of concentrations, but the area is still averaging PM exposure higher than the nation as a whole.
A major obstacle to knowing what kind of PM pollution problems there are is a lack of PM 2.5 monitors in DFW.
 There are currently only four in the entire region and only one in Dallas County. Since PM pollution often comes from very specific local sources, three monitors over more than 10,000 square miles can’t really tell you much about exposure levels in different neighborhoods.
There are currently only four in the entire region and only one in Dallas County. Since PM pollution often comes from very specific local sources, three monitors over more than 10,000 square miles can’t really tell you much about exposure levels in different neighborhoods.
What we do know is that there are plenty of sources for PM pollution in North Texas.
Because DFW is at the crossroads of two major Interstate highways as well as the home to seven million residents, traffic corridors are a constant source of PM pollution. Highway congestion can significantly increase the size, strength and reach of a PM plume. Recent DOT estimates show many parts of central Dallas and Fort Worth are in the top percentile for 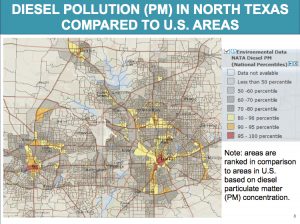 diesel PM pollution exposure.
diesel PM pollution exposure.
These highways often parallel older rail lines that still host PM-spewing diesel locomotives, significantly raising exposure levels near their tracks.
Scattered throughout the western side of DFW are thousands of gas and oil facilities in the Barnett Shale that also release PM pollution. Some are small, but some, such as pipeline compressors, have formidable PM pollution totals ranging from 2 to 20 tons per year.
Regardless of size, their close proximity to homes, schools, and day care centers may result in these oil and gas PM emissions having a disproportional impact on local public health.
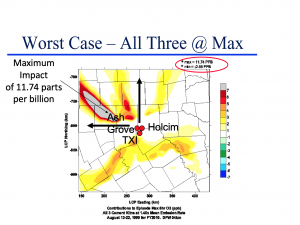
With three large factories in Midlothian, DFW hosts the largest concentration of cement manufacturing in the U.S. Together they release 400 tons of PM a year. Most of the time DFW is downwind of that pollution.
 As freeways were being built in America’s central cities in the 1950’s and 60’s, they often followed existing rail lines and cut a swath through many communities of color living “on the other side of the tracks.”
As freeways were being built in America’s central cities in the 1950’s and 60’s, they often followed existing rail lines and cut a swath through many communities of color living “on the other side of the tracks.”
Tons of PM pollution generated from these traffic corridors falls out primarily in these same communities of color.
Even siting of new sources of PM pollution have followed these old patterns. A look at where the largest PM-emitting gas pipeline compressor stations are located in Fort Worth shows them congregating along major traffic corridors and the central city in predominantly African-American or Mexican-American neighborhoods. There are none on the wealthier West Side – despite it being more gas-rich.
A 2014 UCLA study of Los Angeles found that low-income,  predominantly minority neighborhoods were being exposed to higher PM levels than wealthier and whiter ones. Studies in places as varied as Canada, China, and other cities in the US show the same relationship between income and/or ethnicity and PM exposure.
predominantly minority neighborhoods were being exposed to higher PM levels than wealthier and whiter ones. Studies in places as varied as Canada, China, and other cities in the US show the same relationship between income and/or ethnicity and PM exposure.
Because of this concentrating of people and sources, as well as inequities in health care, the latest research concludes that people of color in the U.S. are significantly more at risk of being harmed by Particulate Matter than their white peers. African-American senior men are three times more likely to die from PM exposure, and African Americans, Asians, Latinos and lower-income seniors all faced generally higher risks of premature death from exposure to PM 2.5 according to the 2017 Harvard study covering 12 years and 95% of the American senior population.
But early death is the bluntest of public health impacts. More nuanced, and maybe more insidious, are the adverse effects to one’s sense of self now tied to PM.
Extrapolating the variety of adverse neurological health impacts caused by PM exposure in the literature, the socioeconomic cause and effect of whole segments of the population breathing poisoned air for decades could be similar to the now well-established link between lead exposure and crime rates in the inner city.
Along with higher-than-average stroke and asthma rates among people of color, increased rates of learning disabilities, graduation failure, and even mental illness could be also attributed to PM pollution. A wide spectrum of behaviors we think of originating by choice or random genetics may actually be instigated by environmental pollution.
PM exposure risks are intertwined with the dusty, archaic land use patterns of segregation and discrimination. Eliminating them melds public health with social justice.
STUDIES ON THE HEALTH HARMS OF PM POLLUTION
“Air pollution can harm acutely, as well as chronically, potentially affecting every organ in the body,” conclude the scientists from the Forum of International Respiratory Societies in the two review papers, published in the journal Chest. “Ultrafine particles pass through the [lungs], are readily picked up by cells, and carried via the bloodstream to expose virtually all cells in the body.
Prof Dean Schraufnagel, at the University of Illinois at Chicago and who led the reviews, said: “I wouldn’t be surprised if almost every organ was affected. If something is missing it is probably because there was no research yet.”
The Short Summary of PM’s Health Effects
CAUSE CHILDREN TO HAVE A LOW IQ: Researchers at the University of California, San Francisco, found in May 2019 that children born to mothers who live in polluted areas have an IQ that is up to seven points lower than those living in places with cleaner air.
CAUSE CHILDREN TO HAVE POORER MEMORY: Researchers at the Barcelona Institute for Global Health found boys exposed to greater levels of PM2.5 in the womb performed worse on memory tests by the time they are 10.
DELAY THE DEVELOPMENT OF CHILDREN: Youngsters who live less than one-third of a mile away from busy roads are twice as likely to score lower on tests of communication skills in infancy, found researchers at Eunice Kennedy Shriver National Institute of Child Health in April. They were also more likely to have poorer hand-eye coordination.
MAKE CHILDREN MORE ANXIOUS: University of Cincinnati scientists claimed pollution may alter the structure of children’s brains to make them more anxious. Their study of 14 youngsters found rates of anxiety was higher among those exposed to greater levels of pollution.
CUT YOUR CHILD’S LIFE SHORT: Children born today will lose nearly two years of their lives because of air pollution, according to a report by the US-based Health Effects Institute and the University of British Columbia in April 2019. UNICEF called for action on the back of the study.
RAISE A CHILD’S RISK OF AUTISM: Researchers at Monash University in Australia discovered youngsters living in highly polluted parts of Shanghai have a 86 per cent greater chance of developing ASD. Lead author Dr Yuming Guo said: ‘The developing brains of young children are more vulnerable to toxic exposures in the environment.’
CAUSE ASTHMA IN CHILDREN: Four million children around the world develop asthma each year because of road traffic pollution, a major study by academics at George Washington University estimated. Experts are divided as to what causes asthma – but exposure to pollution in childhood increases the risk by damaging the lungs.
MAKE CHILDREN FAT: University of Southern California experts found last November that 10 year olds who lived in polluted areas when they were babies are, on average, 2.2lbs (1kg), heavier than those who grew up around cleaner air. Nitrogen dioxide pollution could disrupt how well children burn fat, the scientists said.
LEAVE WOMEN INFERTILE EARLIER: Scientists at the University of Modena, Italy, claimed in May 2019 that they believe pollution speeds up ageing in women, just like smoking, meaning they run out of eggs faster. This was based on them finding almost two-thirds of women who have a low ‘reserve’ of eggs regularly inhaled toxic air.
RAISE THE RISK OF A MISCARRIAGE: University of Utah scientists found in January that pregnant women are 16 per cent more likely to suffer the heartbreak of a miscarriage if they live in areas of high pollution.
RAISE THE RISK OF BREAST CANCER: Scientists at the University of Stirling found six women working at the same bridge next to a busy road in the US got breast cancer within three years of each other. There was a one in 10,000 chance the cases were a coincidence, the study said. It suggested chemicals in the traffic fumes caused the cancer by shutting down the BRCA genes, which try to stop tumours growing.
DAMAGE A MAN’S SPERM: Brazilian scientists at the University of Sao Paulo found in March that mice exposed to toxic air had lower counts and worse quality sperm compared to those who had inhaled clean air since birth.
MAKE MEN LESS LIKELY TO GET SEXUALLY AROUSED: Scientists at Guangzhou Medical University in China found rats exposed to air pollution struggled to get sexually aroused. Scientists believe it may also affect men, as inhaling poisonous particles may trigger inflammation in blood vessels and starve the genitals of oxygen – affecting men’s ability to become sexually aroused.
MAKE MEN MORE LIKELY TO HAVE ERECTILE DYSFUNCTION: Men who live on main roads are more likely to have difficulty getting an erection due to exposure to pollution, a Guangzhou University in China study suggested in February. Toxic fumes reduced blood flow to the genitals, tests on rats showed, putting them at risk of developing erectile dysfunction.
RAISE THE RISK OF PSYCHOSIS: In March, King’s College London scientists linked toxic air to intense paranoia and hearing voices in young people for the first time. They said uncovering exactly how pollution may lead to psychosis should be an ‘urgent health priority’.
MAKE YOU DEPRESSED: Massachusetts Institute of Technology researchers found in January that that the more polluted the air, the sadder we are. Their study was based on analysing social media users in China alongside the average daily PM2.5 concentration and weather data where they lived.
CAUSE DEMENTIA: Air pollution could be responsible for 60,000 cases of dementia in the UK, researchers from King’s College London and St George’s, University of London, calculated last September. Tiny pollutants breathed deep into the lungs and enter the blood stream, where they may travel into the brain and cause inflammation – a problem which may trigger dementia.
Summaries and Links of Individual Studies
LOSS OF IQ
1. “The impact of exposure to air pollution on cognitive performance” Proceedings of the National Academy of Sciences of the United States of America PNAS September 11, 2018 https://doi.org/10.1073/pnas.1809474115
“We find that long-term exposure to air pollution impedes cognitive performance in verbal and math tests. We provide evidence that the effect of air pollution on verbal tests becomes more pronounced as people age, especially for men and the less educated. The damage on the aging brain by air pollution likely imposes substantial health and economic costs, considering that cognitive functioning is critical for the elderly for both running daily errands and making high-stake decisions.”
2. “Socioeconomic Disparities and Sexual Dimorphism in Neurotoxic Effects of Ambient Fine Particles on Youth IQ: A Longitudinal Analysis” (PLOS ONE) December 5, 2017 http://healthpolicy.ucla.edu/publications/search/pages/detail.aspx?PubID=1707
“Mounting evidence indicates that early-life exposure to particulate air pollutants pose threats to children’s cognitive development, but studies about the neurotoxic effects associated with exposures during adolescence remain unclear. Study authors examined whether exposure to ambient fine particles (PM2.5) at residential locations affects intelligence quotient (IQ) during pre-/early- adolescence (ages 9-11) and emerging adulthood (ages 18-20) in a demographically-diverse population (N = 1,360) residing in Southern California. Increased ambient PM2.5 levels were associated with decreased IQ scores. This association was more evident for Performance IQ (PIQ), but less for Verbal IQ, assessed by the Wechsler Abbreviated Scale of Intelligence.”
3. “Air pollution can affect memory and IQ“ Journal of Alzheimer’s Disease, February 18, 2015 https://pdfs.semanticscholar.org/e3d5/8109827f3020c60a1efef6db47f494072bac.pdf
“….two groups of children living in Mexico City were compared including multiple variables, such as age, gender, socioeconomic status and education, among others. Then, differences between children carrying the variant epsilon 4 with carriers of the epsilon 3 variant were analyzed. They found that the former had three notable changes: They showed short-term memory deficits, an IQ within the normal limits but 10 average points lower, and key metabolic changes in the brain, which resemble those of people with Alzheimer’s disease.”
DIABETES
1. “The 2016 global and national burden of diabetes mellitus attributable to PM2·5 air pollution” The Lancet Volume 2, ISSUE 7, Pe301-e312, July 01, 2018 https://www.thelancet.com/journals/lanpla/article/PIIS2542-5196(18)30140-2/fulltext
“The global toll of diabetes attributable to PM2·5 air pollution is significant. Reduction in exposure will yield substantial health benefits.”
2. “Air Pollution as a Risk Factor for Type 2 Diabetes” US National Library of Medicine, National Institutes of Health 2015 Feb https://www.ncbi.nlm.nih.gov/pmc/articles/PMC4306726/
3. “From the University of Maryland comes a report that concludes air pollution increases inflamation of the heart which leads to diabetes when combined with a high fat diet – the kind so many Americans are still eating. Sedentary mice were fed the high-fat diet and then forced to breath Beijing-like levels of air pollution. Exposure to that bad air, primarily high levels of particulate matter, increased the likelihood of the mice developing diabetes by 2 to 4 times, and increased he severity of the disease as well. “
MENTAL ILLNESS
1. “Spatiotemporal influence of temperature, air quality, and urban environment on cause-specific mortality during hazy days” Environment International Volume 112, March 2018, Pages 10-22 https://www.ncbi.nlm.nih.gov/pubmed/29245038
“A Hong Kong university study published in the upcoming March edition of Environment International concludes the risk of death for people with mental and behavioral disorders rises sharply on days when particulate matter and other kinds of air pollution reaches toxic peaks. Reviewing a decade of death statistics revealed a 16% increase in mortality risk on the first day of haze and a 27% increase on the second day compared to better air days. If the haze was accompanied by high ozone pollution, the risk of death increased by 79%.”
2.”Association between neighbourhood air pollution concentrations and dispensed medication for psychiatric disorders in a large longitudinal cohort of Swedish children and adolescents” BMJ OPEN Volume 6, Issue 6 https://bmjopen.bmj.com/content/6/6/e010004.full
This Swedish study is the first to report linking air pollution to mental illness in children. It found that relatively small increases in air pollution were associated with a significant increase in treated psychiatric problems.
3. Air pollution exposure linked to bipolar disorder, schizophrenia and depression “Environmental pollution is associated with increased risk of psychiatric disorders in the US and Denmark”
Plos Biology, August 20, 2019 https://journals.plos.org/plsbiology/article?id=10.1371/journal.pbio.3000353
“These results show that air pollution is significantly associated with increased risk of psychiatric disorders. We hypothesize that pollutants affect the human brain via neuroinflammatory pathways that have also been shown to cause depression-like phenotypes in animal studies.”
ANTI-SOCIAL BEHAVIOR/CRIME
1.”Longitudinal Analysis of Particulate Air Pollutants and Adolescent Delinquent Behavior in Southern California” Journal of Abnormal Child Psychology, August 2018, Volume 46, Issue 6, pp 1283-1293https://link.springer.com/article/10.1007/s10802-017-0367-5
“The first study to look at the effects of PM pollution exposure on the social behavior of children found that that the more bad air a child inhaled, the more likely they were to engage in delinquent activity. “
“Multilevel mixed-effects models were used to examine the association between PM2.5 exposure and individual trajectories of delinquent behavior, adjusting for within-family/within-individual correlations and potential confounders. The results sμggest that PM2.5 exposure at baseline and cumulative exposure during follow-up was significantly associated (p < 0.05) with increased delinquent behavior.”
2.“Traffic-Related Air Pollution Exposure in the First Year of Life and Behavioral Scores at 7 Years of Age “ Environmental Health Perspectives June 1 2013 https://ehp.niehs.nih.gov/doi/10.1289/ehp.1205555
“We explored the association between early-life exposure to TRAP using a surrogate, elemental carbon attributed to traffic (ECAT), and attention deficit/hyperactivity disorder (ADHD) symptoms at 7 years of age. Results: Exposure to the highest tertile of ECAT during the child’s first year of life was significantly associated with Hyperactivity T-scores in the “at risk” range at 7 years of age, after adjustment [adjusted odds ratio (aOR) = 1.7; 95% CI: 1.0, 2.7]. Stratification by maternal education revealed a stronger association in children whose mothers had higher education (aOR = 2.3; 95% CI: 1.3, 4.1).” Conclusions: ECAT exposure during infancy was associated with higher Hyperactivity scores in children; this association was limited to children whose mothers had more than a high school education.”
3.“Prenatal and childhood traffic-related air pollution exposure and childhood executive function and behavior.”
Neurotoxicol Teratol. Sept2016https://www.ncbi.nlm.nih.gov/pubmed/27350569
“Traffic-related air pollution exposure may influence brain development and function and thus be related to neurobehavioral problems in children, but little is known about windows of susceptibility. Using validated spatiotemporal models, we estimated exposure to black carbon (BC) and fine particulate matter (PM2.5) in the third trimester of pregnancy, from birth to 3 years, from birth to 6 years, and in the year before behavioral ratings. We also measured residential distance to major roadways and near-residence traffic density at birth and in mid-childhood. We estimated associations of BC, PM2.5, and other traffic exposure measures with BRIEF and SDQ scores, adjusted for potential confounders. Children with higher mid-childhood exposure to BC and greater near-residence traffic density in mid-childhood had greater problems with behavioral regulation as assessed by classroom teachers, but not as assessed by parents.”
4. “Acute air pollution exposure and the risk of violent behavior in the United States”
Berman, Jesse Da; Burkhardt, Jesseb; Bayham, Judeb; Carter, Ellisonc; Wilson, AnderdEpidemiology: August 12, 2019 – Volume Publish Ahead of Print – Issue – p https://journals.lww.com/epidem/Abstract/publishahead/Acute_air_pollution_exposure_and_the_risk_of.98514.aspx
“Our results suggest that short-term changes in ambient air pollution may be associated with greater risk of violent behavior, regardless of community type.”
5. “The effect of pollution on crime: Evidence from data on particulate matter and ozone”
Journal of Environmental Economics and Management Volume 98, November 2019, 102267
“We find a robust positive effect of increased air pollution on violent crimes, and specifically assaults, but no relationship between increases in air pollution and property crimes. The effects are present in and out of the home, at levels well below Ambient Air Pollution Standards, and PM2.5 effects are strongest at lower temperatures. The results suggest that a 10% reduction in daily PM2.5 and ozone could save $1.4 billion in crime costs per year, a previously overlooked cost associated with pollution.”
BRAIN DISEASE/DEMENTIA
1.“Long-Term Exposure to Fine Particulate Matter, Residential Proximity to Major Roads and Measures of Brain Structure” STROKE American Heart Association Journal April 3 2015
https://www.ahajournals.org/doi/full/10.1161/STROKEAHA.114.008348
“Exposure to elevated levels of PM2.5 was associated with smaller total cerebral brain volume, a marker of age-associated brain atrophy, and with higher odds of covert brain infarcts. These findings suggest that air pollution is associated with insidious effects on structural brain aging even in dementia- and stroke-free persons.”
2. “Particulate air pollutants, APOE alleles and their contributions to cognitive impairment in older women and to amyloidogenesis in experimental models” Translational Psychiatry January 31 2017
“University of Southern California researchers looked at over 1,400 women without dementia who were initially enrolled in a large health study from 1996 to 1998. Researchers measured their brain volume with M.R.I. scans in 2005 and 2006, when the women were 71 to 89 years old.”
“Using residential histories and air pollution monitoring data, they estimated their exposure to PM air pollution from 1999 to 2006. For each increase of 3.49 micrograms per cubic centimeter (μg/m3) cumulative exposure to PM, there was an associated 6.23 cubic centimeter reduction in the subject’s brain white matter, the equivalent of one to two years of brain aging. The current EPA standard for 24 PM exposure is 35 μg/m3, while the annual average standard is 12 μg/m3, although many leading scientists now believe there’s no “safe” level of exposure to PM pollution. That is, any amount of exposure is capable of doing some damage.”
3. “The emerging risk of exposure to air pollution on cognitive decline and Alzheimer’s disease – Evidence from epidemiological and animal studies” Biomedical Journal Published online 2018 Jul 17 https://www.ncbi.nlm.nih.gov/pubmed/30080655
“In this review, we summarize recent evidence supporting exposure to air pollution as a risk for cognitive decline at all ages and AD at later lifetime. Additionally, we review the current body of work investigating the molecular mechanisms by which air pollutants mediate damage in the CNS.”
4. “Fine Particulate Matter Air Pollution and Cognitive Function Among U.S. Older Adults” The Journals of Gerontology March 2015 https://www.ncbi.nlm.nih.gov/pmc/articles/PMC4351385/
“In a study involving approximately 15,000 people, the U.S. National Institute on Aging found that higher levels of exposure to fine particulate matter pollution, or soot, is prematurely aging the brain of those 50 and older by up to three years.”
5. “Non-Phosphorylated Tau in Cerebrospinal Fluid is a Marker of Alzheimer’s Disease Continuum in Young Urbanites Exposed to Air Pollution” Journal of Alzheimer’s Disease, vol. 66, no. 4, pp. 1437-1451, 2018 https://content.iospress.com/articles/journal-of-alzheimers-disease/jad180853
“Long-term exposure to fine particulate matter (PM2.5) and ozone (O3) above USEPA standards is associated with Alzheimer’s disease (AD) risk.”
AUTISM
1.”Echoes of Autism? Inhaled Ultrafine Particles and Brain Changes in Mice”
Environmental Health Perspectives, September 2014
https://www.ncbi.nlm.nih.gov/pmc/articles/PMC4154204/
“Epidemiological evidence has raised the possibility that exposure to air pollution could be a risk factor for autism spectrum disorders (ASDs) and schizophrenia. The team, led by Deborah Cory-Slechta of the University of Rochester Medical Center (URMC), found that exposure to ultrafine particles early in life produced brain changes in mice suggestive of those in humans with ASDs and schizophrenia. Notably, the brains of exposed male mice showed enlarged lateral ventricles, a condition called ventriculomegaly. “That’s alarming, because ventriculomegaly in humans has behavioral consequences” including ASDs6 and schizophrenia, says Cory-Slechta.”
2. “Perinatal Air Pollutant Exposures and Autism Spectrum Disorder in the Children of Nurses’ HealthStudy II Participants” Environmental Health Perspectives June 18, 2013 https://ehp.niehs.nih.gov/doi/10.1289/ehp.1206187
“We estimated associations between U.S. Environmental Protection Agency-modeled levels of hazardous air pollutants at the time and place of birth and ASD in the children of participants in the Nurses’ Health Study II (325 cases, 22,101 controls). For most pollutants, associations were stronger for boys (279 cases) than for girls (46 cases) and significantly different according to sex. Conclusions: Perinatal exposure to air pollutants may increase risk for ASD.”
“Women in the U.S. exposed to high levels of air pollution while pregnant were up to twice as likely to have a child with autism as women who lived in areas with low pollution, according to a new study from Harvard School of Public Health (HSPH). It is the first large national study to examine links between autism and air pollution across the U.S.”
“What you see is the mothers with the 20 percent least exposure to pollutants, their children are least likely to have autism,” lead researcher Dr. Andrea Roberts of the Harvard School of Public Health told The Standard-Times. “With each percentile of pollutant exposure, the presence of autism increased.”
3. “Autism Spectrum Disorder and Particulate Matter Air Pollution before, during, and after Pregnancy: A Nested Case-Control Analysis within the Nurses’ Health Study II Cohort” Environmetnal Health Perspectives August 2015 https://ehp.niehs.nih.gov/doi/10.1289/ehp.1408133
“We explored the association between maternal exposure to particulate matter (PM) air pollution and odds of ASD in her child. The association between ASD and PM2.5 was stronger for exposure during the third trimester (OR = 1.42 per IQR increase in PM2.5; 95% CI: 1.09, 1.86) than during the first two trimesters (ORs = 1.06 and 1.00) when mutually adjusted. Conclusions: Higher maternal exposure to PM2.5 during pregnancy, particularly the third trimester, was associated with greater odds of a child having ASD.”
4. “Residential Proximity to Freeways and Autism in the CHARGE Study” Environmeental Health Perspectives March 1 2013 https://www.ncbi.nlm.nih.gov/pmc/articles/PMC3114825/
“The more Ozone and Particulate Matter pollution a baby in the womb is exposed to, the more likely he or she will be born with autism according to a new UCLA study
![]()
. It’s the largest study of its kind to date and is the first to link autism with ozone, or smog, levels.”
“Researchers compared levels of air pollutants, mostly related to vehicle traffic, during pregnancy gestation periods of 7,603 children with autism and 75,635 children without autism, born from 1995 to 2006 in Los Angeles. Babies at the 75th percentile of exposure to toxins had a 8 percent to 10 percent higher risk of autism than babies at the bottom 25th percentile, the study said. Ozone and fine particulates had the strongest association with autism.”
5. “Early life exposure to particulate matter air pollution (PM1, PM2.5and PM10) and autism in Shanghai, China: A case-control study.” Environment International Volume 121, Part 2, December 2018
https://www.sciencedirect.com/science/article/pii/S0160412018313242?via%3Dihub
“A case-control study was performed in Shanghai with a multi-stage random sampling design. Children’s exposures to PM1, PM2.5 and PM10 (particulate matter with aerodynamic diameter < 1 μm, < 2.5 μm and < 10 μm, respectively) during the first three years after birth were estimated with satellite remote sensing data. Conditional logistic regression was used to examine the PM-ASD association.”
“Conclusions: Exposures to PM1, PM2.5 and PM10 during the first three years of life were associated with the increased risk of ASD and there appeared to be stronger effects of ambient PM pollution on ASD in the second and the third years after birth.”
HEART DISEASE/ATTACKS
1. “Association Between Ambient Air Pollution and Cardiac Morpho-Functional Phenotypes” Circulation Vol 138 No 20 August 2, 2018 https://www.ahajournals.org/doi/full/10.1161/CIRCULATIONAHA.118.034856
“Exposure to ambient air pollution is strongly associated with increased cardiovascular morbidity and mortality. Little is known about the influence of air pollutants on cardiac structure and function. We aim to investigate the relationship between chronic past exposure to traffic-related pollutants and the cardiac chamber volume, ejection fraction, and left ventricular remodeling patterns after accounting for potential confounders.”
“Conclusions: In a large asymptomatic population with no prevalent cardiovascular disease, higher past exposure to particulate matter with an aerodynamic diameter <2.5 µm and nitrogen dioxide was associated with cardiac ventricular dilatation, a marker of adverse remodeling that often precedes heart failure development.”
“We found that as PM 2.5 exposure rises, the larger the heart gets and the worse it performs. Both of these measures are associated with increased morbidity and mortality from heart disease.”
2. “Combustion- and friction-derived magnetic air pollution nanoparticles in human hearts” Environmental Research Volume 176, September 2019, 108567
https://www.sciencedirect.com/science/article/pii/S0013935119303640
“Iron-rich, strongly magnetic combustion- and friction-derived nanoparticles are present in abundance in young urbanites’ hearts. Mexico City residents have up to ∼22 billion magnetic NPs/g of ventricular tissue.. Oxidative and endoplasmic reticulum (ER) stress are significant in human ventricular tissues. Exposure to solid NPs appears to be directly associated with early and significant cardiac damage.”
3. “Air Pollution Exposure and Cardiovascular Disease”
Toxicological Research, June 30 2014 https://www.ncbi.nlm.nih.gov/pmc/articles/PMC4112067/
“Ambient air pollution (AAP) and particulate matters (PM) have been closely associated with adverse health effects such as respiratory disease and cardiovascular diseases. Previous studies have examined the adverse health effects associated with short- and long-term exposure to AAP and outdoor PM on respiratory disease. Both PM2.5and PM10 air pollution concentrations have a marked and close association with adverse health effect, such as heart disease, stroke, blood pressure, and cardiovascular diseases. Nevertheless, epidemiological studies exhibit a stronger correlation of adverse health effects with PM2.5 than with PM10. “
4. “Air Pollution and Cardiovascular Disease A JACC State-of-the-Art Review”, Journal of the American College of Cardiology October 17, 2018 http://www.onlinejacc.org/content/72/17/2054
“Fine particulate matter <2.5 μm (PM2.5) air pollution is the most important environmental risk factor contributing to global cardiovascular (CV) mortality and disability. Short-term elevations in PM2.5 increase the relative risk of acute CV events by 1% to 3% within a few days. Longer-term exposures over several years increase this risk by a larger magnitude (∼10%), which is partially attributable to the development of cardiometabolic conditions (e.g., hypertension and diabetes mellitus). As such, ambient PM2.5 poses a major threat to global public health.
5. “Association of ambient particulate matter with heart failure incidence and all-cause readmissions in Tasmania: an observational study”
BMJ Journals BMJ Open Volume 8, Issue 5 https://bmjopen.bmj.com/content/8/5/e021798
“PM2.5 was detrimentally associated with HF incidence (risk ratio (RR)=1.29 (1.15-1.42)) and weakly so with readmission (RR=1.07 (1.02-1.17)), with 1 day time lag. In multivariable analyses, PM2.5 significantly predicted HF incidence (RR=1.12 (1.01-1.24)) but not readmission (RR=0.96 (0.89-1.04)). HF incidence was similarly low when PM <4 µg/m3 and only started to rise when PM2.5≥4 µg/m3. Stratified analyses showed that PM2.5 was associated with readmissions among patients not taking beta-blockers but not among those taking beta-blockers (pinteraction=0.011). Conclusions PM2.5 predicted HF incidence, independent of other environmental factors. A possible threshold of PM2.5=4 µg/m3 is far below the daily Australian national standard of 25 µg/m3. Our data suggest that beta-blockers might play a role in preventing adverse association between air pollution and patients with HF.”
6, “Cardiovascular and Cerebrovascular Emergency Department Visits Associated With Wildfire Smoke Exposure in California in 2015” Journal of the Amerian Heart Association, April 18, 2018 https://www.ahajournals.org/doi/10.1161/JAHA.117.007492
“Wildfire smoke is known to exacerbate respiratory conditions; however, evidence for cardiovascular and cerebrovascular events has been inconsistent, despite biological plausibility. Analysis of an extensive wildfire season found smoke exposure to be associated with cardiovascular and cerebrovascular ED visits for all adults, particularly for those over aged 65 years.”
7. “Global association of air pollution and heart failure: a systematic review and meta-analysis” The Lancet July 10, 2013 https://www.thelancet.com/journals/lancet/article/PIIS0140-6736(13)60898-3/fulltext
“Increases in particulate matter concentration were associated with heart failure hospitalisation or death (PM2·5 2·12% per 10 μg/m3, 95% CI 1·42-2·82; PM10 1·63% per 10 μg/m3, 95% CI 1·20-2·07). Strongest associations were seen on the day of exposure, with more persistent effects for PM2·5. In the USA, we estimate that a mean reduction in PM2·5 of 3·9 μg/m3 would prevent 7978 heart failure hospitalisations and save a third of a billion US dollars a year. Air pollution has a close temporal association with heart failure hospitalisation and heart failure mortality. Although more studies from developing nations are required, air pollution is a pervasive public health issue with major cardiovascular and health economic consequences, and it should remain a key target for global health policy. “
LEUKEMIA/CANCER
1. “Residential Traffic Exposure and Childhood Leukemia”
American Journal of Preventive Medicine April 2014 https://www.ajpmonline.org/article/S0749-3797%2813%2900619 3/abstract
“After a review of over 30 years of studies, the Centers for Disease Control concluded that children living near high-volume roads and highways were 50% more likely to suffer from childhood leukemia. The cancer risk is linked to postnatal exposure. Out of nine relevant studies, seven, covering approximately 8,000 children, reveled a correlation between exposure and leukemia.”
2. “The International Agency for Research on Cancer (IARC) evaluation of the carcinogenicity of outdoor air pollution: focus on China.”
Chinese Journal of Cancer April 2014 https://www.ncbi.nlm.nih.gov/pubmed/24694836
“The air you breathe CAN kill you, at least according to the World Health Organization, which officially classified air pollution as a cause of lung cancer. The move came after the group released a report earlier this year estimating that over 220,000 people died from lung cancer worldwide from exposure to bad air. Most of those deaths are occurring in countries in Asia. Mostly these deaths are due to Particulate Matter pollution, the ubiquitous tiny particles of soot that are produced when things burn, like gas in cars, coal or gas or waste in power plants and cement kilns, and diesel engines and flares in the the gas fields.”
3. “Air pollution and lung cancer incidence in 17 European cohorts: prospective analyses from the European Study of Cohorts for Air Pollution Effects” The Lancet July 10, 2013 https://www.thelancet.com/journals/lanonc/article/PIIS1470-2045(13)70279-1/fulltext
“Interpretation: Particulate matter air pollution contributes to lung cancer incidence in Europe. Lung cancer risks went up 18% with each increase of 5 migrograms of PM 2.5. Researchers noted that they did not find a level of pollution for where there was no risk, and the results indicated “the more the worse, the less the better” when it came to pollution.”
NEONATAL
1.“Air pollution linked to increase in newborn intensive care admissions”
Annals of Epidemiology. July 19, 2019
https://www.sciencedirect.com/science/article/abs/pii/S1047279719300572
“Infants born to women exposed to high levels of air pollution ((pollution particles less than 2.5 microns in diameter or PM2.5 ) in the week before delivery are more likely to be admitted to a newborn intensive care unit (NICU). ‘Short-term exposure to most types of air pollutants may increase the risk for NICU admission,’ Dr. Mendola said. “If our findings are confirmed, they suggest that pregnant women may want to consider limiting their time outdoors when air quality advisories indicate unhealthy conditions. Depending on the type of pollution, chances for NICU admission increased from about 4% to as much as 147%, compared to infants whose mothers did not encounter high levels of air pollution during the week before delivery. “
2. “Ambient air pollution and the risk of pregnancy loss: a prospective cohort study”
January 2018Volume 109, Issue 1, Pages 148-153 https://www.fertstert.org/article/S0015-0282(17)31973-8/fulltext
“Average chronic whole pregnancy exposures to ozone and PM2.5 were positively associated with the risk of pregnancy loss. An IQR increase (from the 25th to 75th percentile) in ozone and PM2.5 exposures were, respectively, associated with a 12% (HR 1.12, 95% CI 1.07-1.17), and 13% (HR 1.13, 95% CI 1.13-1.24) increased risk of pregnancy loss. These findings suggest that chronic exposure may be more detrimental than acute exposures during sensitive windows.”
3. “Impact of London’s road traffic air and noise pollution on birth weight: retrospective population based cohort study”
The British Medical Journal 05 December 2017 https://www.bmj.com/content/359/bmj.j5299 “The findings suggest that air pollution from road traffic in London is adversely affecting fetal growth. To our knowledge, this is the largest UK study on air pollution and birth weight, and the first UK study and largest study worldwide of birth weight and noise exposure. We observed that long term exposure during pregnancy to NO2, NOx, PM2.5 overall and specifically from traffic exhaust and non-exhaust sources, and PM10, were all associated with increased risk of LBW at term, across London. Our findings from two air pollutant models suggest that associations between term LBW and air pollutants emitted from vehicle exhausts may be driven by the fine particulate matter (PM2.5 traffic exhaust) component rather than the gaseous NOx component. “
4.”Exposures to fine particulate matter (PM2.5) and birthweight in a rural-urban, mother-child cohort in Tamil Nadu, India.”
Environmental Research Volume 161, February 2018, https://www.sciencedirect.com/science/article/pii/S0013935117312276?via%3Dihub
“Results: A 10-μg/m3 increase in pregnancy period PM2.5 exposures was associated with a 4 g (95% CI: 1.08 g, 6.76 g) decrease in birthweight and 2% increase in prevalence of low birthweight [odds ratio(OR) = 1.02; 95%CI:1.005,1.041] after adjusting for gestational age, infant sex, maternal BMI, maternal age, history of a previous low birth weight child, birth order and season of conception.
Conclusions: The study provides some of the first quantitative effects estimates for linking rural-urban PM2.5exposures and birthweight in India, adding important evidence for this association from high exposure settings in LMICs, that also experience dual health burdens from ambient and household air pollution. Study results also point to the need for considering maternal PM2.5exposures alongside other risk factors for low birthweight in India.”
5. “The association between air pollution and preterm birth and low birth weight in Guangdong, China ” BMC Public Healthvolume 19, Article number: 3 (2019) https://bmcpublichealth.biomedcentral.com/articles/10.1186/s12889-018-6307-7
“A mountain of evidence has shown that people’s physical and mental health can be affected by various air pollutions. Poor pregnancy outcomes are associated with exposure to air pollution. Therefore, this study aims to investigate the association between air pollutions (PM2.5, PM10, SO2, NO2, CO, and O3) and preterm birth/low birth weight in Guangdong province, China. Conclusion: This study provides further evidence for the relationships between air pollutions and preterm birth/low birth weight. Pregnant women are recommended to reduce or avoid exposure to air pollutions during pregnancy, especially in the early and late stages of pregnancy.”
6. “Ambient PM2.5 and birth outcomes: Estimating the association and attributable risk using a birth cohort study in nine Chinese cities”
Environment International Volume 126, May 2019, Pages 329-335
https://www.sciencedirect.com/science/article/pii/S0160412018326473
“We examined associations in a birth cohort of 1,455,026 mother-and-live-birth pairs who were followed up from the first hospital visit for pregnancy until the birth of the baby during 2014-2017 in nine cites of the Pearl River Delta (PRD) region, China. The PM2.5 exposures were estimated based on the air pollution concentrations of the nearby monitors. Cox proportional hazards regressions were employed to examine the associations. The results indicate that maternal PM2.5 exposure is a risk factor for both LBW and PTB, and responsible for considerable burdens of PTB and LBW in the Pearl River Delta region.”
7. “Ambient Fine Particulate Matter, Nitrogen Dioxide, and Term Birth Weight in New York, New York “ American Journal of Epidemiology, Volume 179, Issue 4, 15 February 2014, Pages 457-466, https://academic.oup.com/aje/article/179/4/457/127797
“Using NYCCAS air monitoring data, the research team examined to the associations of PM2.5 and NO2 in ambient air with birth weights of 252,967 babies born to New York City mothers at full term from 2008-2010. Our results add support to the possible impact of common air pollutants, specifically PM2.5 and nitrogen dioxide, on fetal growth. The results of this study showed that for every of 10-µg/m3 increase in PM2.5 exposure over the entire pregnancy, birth weight was reduced by 48.4 g. Similarly, results show that for every 10-ppb increase in NO2 exposure over the entire pregnancy, birth weights were reduced by 18.0 g.”
8. “Exposure to Ambient Particulate Matter during Specific Gestational Periods Produces Adverse Obstetric Consequences in Mice”
Environmental Health Perspectives.July 27, 2017 https://ehp.niehs.nih.gov/doi/10.1289/EHP1029
“The study, conducted in mice, found that exposure to air pollution during the equivalent of the first or second trimester in humans was linked to more negative birth outcomes than exposure later in pregnancy. Researchers studied the effects of fine particulate air pollution, which is made up of particles less than one ten-thousandth of an inch in diameter, or PM2.5. Inhalable and almost invisible to the eye, this type pollution comes from car exhaust, coal-fired power plants, and other industrial processes. PM2.5exposure has previously been linked to risk for asthma and heart disease. According to the US Centers for Disease Control and Prevention, preterm birth and low birth weight increase risk for vision and hearing problems, learning problems and even death.”
9. “Pre-conception Exposure to Air Pollution and Risk of Congenital Malformations” The Journal of Pediatrics September 2017 https://www.jpeds.com/article/S0022-3476(17)31330-6/fulltext
“Using birth certificate data from the Ohio Department of Health (2006-2010) and PM2.5 data from the US Environmental Protection Agency’s 57 monitoring stations located throughout Ohio, the geographic coordinates of the mother’s residence for each birth were linked to the nearest PM2.5 monitoring station and monthly exposure averages were calculated. Conclusions: Increased exposure to PM2.5 in the periconception period is associated with some modest risk increases for congenital malformations. The most susceptible time of exposure appears to be the 1 month before and after conception. Although the increased risk with PM2.5 exposure is modest, the potential impact on a population basis is noteworthy because all pregnant women have some degree of exposure.”
10. Air pollution exposure associates with increased risk of neonatal jaundice
https://www.nature.com/articles/s41467-019-11387-3
NATURE, Published: 20 August 2019
“Clinical experience suggests increased incidences of neonatal jaundice when air quality worsens, yet no studies have quantified this relationship. Here we reports investigations in 25,782 newborns showing an increase in newborn’s bilirubin levels, the indicator of neonatal jaundice risk, by 0.076 (95% CI: 0.027-0.125), 0.029 (0.014-0.044) and 0.009 (95% CI: 0.002-0.016) mg/dL per μg/m3 for PM2.5 exposure in the concentration ranges of 10-35, 35-75 and 75-200 μg/m3, respectively. The response is 0.094 (0.077-0.111) and 0.161 (0.07-0.252) mg/dL per μg/m3 for SO2 exposure at 10-15 and above 15 μg/m3, respectively, and 0.351 (0.314-0.388) mg/dL per mg/m3 for CO exposure. Bilirubin levels increase linearly with exposure time between 0 and 48 h. Positive relationship between maternal exposure and newborn bilirubin level is also quantitated. The jaundice−pollution relationship is not affected by top-of-atmosphere incident solar irradiance and atmospheric visibility. Improving air quality may therefore be key to lowering the neonatal jaundice risk.”
EARLY DEATH
1. “Associations of PM2.5 Constituents and Sources with Hospital Admissions: Analysis of Four Counties in Connecticut and Massachusetts (USA) for Persons ≥ 65 Years of Age”
Environmental Health Perspectives Vol. 122, No. 2 February 2014
https://ehp.niehs.nih.gov/doi/10.1289/ehp.1306656
“Results: PM2.5 total mass and PM2.5 road dust contribution were associated with cardiovascular hospitalizations, as were the PM2.5 constituents calcium, black carbon, vanadium, and zinc. For respiratory hospitalizations, associations were observed with PM2.5 road dust, and sea salt as well as aluminum, calcium, chlorine, black carbon, nickel, silicon, titanium, and vanadium.”
“Our work indicates that some constituents of PM2.5 may be more toxic than others and therefore regulating PM total mass alone may not be sufficient to protect human health,” the authors wrote in Environmental Health Perspectives.”
2. “New evidence on the impact of sustained exposure to air pollution on life expectancy from China’s Huai River Policy”
Proceedings of the National Academy of Science September 11, 2017 https://www.pnas.org/content/early/2017/09/05/1616784114.full ‘”This paper finds that a 10-μg/m3 increase in airborne particulate matter [particulate matter smaller than 10 μm (PM10)] reduces life expectancy by 0.64 years (95% confidence interval = 0.21-1.07). Furthermore, the shorter lifespans are almost entirely caused by elevated rates of cardiorespiratory mortality, suggesting that PM10 is the causal factor. The estimates imply that bringing all of China into compliance with its Class I standards for PM10 would save 3.7 billion life-years.”
3. “Particulate matter air pollution and national and county life expectancy loss in the USA: A spatiotemporal analysis”
PLOS Medicine July 23, 2019 https://doi.org/10.1371/journal.pmed.1002856
“Exposure to fine particulate matter pollution (PM2.5) is hazardous to health. Our aim was to directly estimate the health and longevity impacts of current PM2.5 concentrations and the benefits of reductions from 1999 to 2015, nationally and at county level, for the entire contemporary population of the contiguous United States.”
“PM2.5 pollution in excess of the lowest observed concentration (2.8 μg/m3) was responsible for an estimated 15,612 deaths (95% credible interval 13,248-17,945) in females and 14,757 deaths (12,617-16,919) in males. These deaths would lower national life expectancy by an estimated 0.15 years (0.13-0.17) for women and 0.13 years (0.11-0.15) for men. The life expectancy loss due to PM2.5 was largest around Los Angeles and in some southern states such as Arkansas, Oklahoma, and Alabama. At any PM2.5 concentration, life expectancy loss was, on average, larger in counties with lower income and higher poverty rate than in wealthier counties.“
4. Air pollution can kill, even when it meets air quality guidelines “Ambient Particulate Air Pollution and Daily Mortality in 652 Cities” New England Journal of Medicine, August 22, 2019
“We evaluated the associations of inhalable particulate matter (PM) with an aerodynamic diameter of 10 μm or less (PM10) and fine PM with an aerodynamic diameter of 2.5 μm or less (PM2.5) with daily all-cause, cardiovascular, and respiratory mortality across multiple countries or regions. The pooled concentration-response curves showed a consistent increase in daily mortality with increasing PM concentration, with steeper slopes at lower PM concentrations.”
Blindness
1.Air Pollution From Cars Linked to Degenerative Eye Disease
https://gizmodo.com/air-pollution-from-cars-linked-to-degenerative-eye-dise-1837382732
https://jim.bmj.com/content/early/2019/07/11/jim-2019-001007
Traffic-related air pollutants increase the risk for age-related macular degeneration
“The aim of this study was to investigate whether ambient nitrogen dioxide (NO2) and carbon monoxide (CO) increase the risk for age-related macular degeneration (AMD). Compared with the lowest exposure quartile, the highest quartile of each air pollutant was associated with an increased risk for AMD. In this study, chronic exposure to the highest quartile of ambient NO2 or CO significantly increases the risk for AMD.”
2. “The Relationship Between Ambient Atmospheric Fine Particulate Matter (PM2.5) and Glaucoma in a Large Community Cohort”
Investigative Ophthalmology & Visual Science November 2019, Vol.60, 4915-4923. doi:https://doi.org/10.1167/iovs.19-28346
“Greater exposure to PM2.5 is associated with both self-reported glaucoma and adverse structural characteristics of the disease. The absence of an association between PM2.5 and IOP suggests the relationship may occur through a non-pressure-dependent mechanism, possibly neurotoxic and/or vascular effects.”